The life and times of a pituitary Cushing's survivor (1987) AND a kidney cancer (Renal Cell Carcinoma) survivor (2006). I must be a Super-Woman...NOT!
Friday, October 31, 2008
A great Blog Post from "Dr. Rob"
Read it all here: Dealing with Hardship
My job involves being around people who are struggling. Many people are dealing with personal illness, while others with loss. Whatever the case, it is a very common occurrence to sit alongside of someone who is in significant hardship.
Here is my advice to them, and to you if you are dealing with difficulty:
- You can cry in front of me. If there is anyone you can cry in front of, it is your doctor...
- Most of the people around you don’t know what to do... Be patient with them. The people closest to you are often the most awkward.
- It’s OK to lie. When people see you socially and say, “How are you doing?” they don’t really want to know; they are just being polite...
- People will say really stupid things to you... Just tell yourself that they are idiots, and ignore what they say.
- Depression is irrational... The nature of depression is to be out of control of your emotions, so don’t feel like you are crazy when this happens.
- Being happy does not mean you are not sad... Good things don’t negate the bad. There cannot be silver linings without dark clouds.
- Try not to isolate yourself...
- There are two kinds of depression...
- It is normal for depressed people to wish they are dead...
- Time helps. Life is full of hard things to lots of people...
- Don’t protect your loved ones...
- If you need me, please bug me.
Thanks for these, Dr. Rob! Be sure to read the whole post at http://distractible.org/2008/10/30/dealing-with-hardship/
How to Cure Your Kidney Cancer: Some Methods
http://allaboutkidney.blogspot.com/2008/10/how-to-cure-your-kidney-cancer-some.html
Surgically getting rid of the affected kidney gives a reasonable possibility of cure if the cancer has not spread outside the kidney. On the other hand, surgeons might eliminate merely the tumor with a rim of neighboring normal tissue, which spares the residue of the kidney.
Kidney cancer, however, has a propensity to extend early, particularly to the lungs, occasionally prior to symptoms progress. Since kidney cancer that has extended to distant locations might escape early diagnosis, metastasis at times becomes apparent simply after doctors have surgically eliminated all of the kidney cancer that can be gotten.
Between 80 and 90% of patients can be cured if the cancer is diagnosed at an early phase, earlier than it has extended beyond the kidney. But if the tumour spreads beyond the kidney, it is more complicated to deal with. Advanced kidney cancer is so hard to cure totally and simply roughly one in six or seven patients can be cured.
Cryotherapy is a technique of killing cancer cells by freezing them. Some doctors state that the benefit of utilizing cryotherapy is that it might offer the possibility of cure with no the risks of having to remove a kidney. However they have to follow up patients for longer to ensure that cryotherapy gives as good a cure rate as surgery does. A number of researches propose that kidney cancer may be more probable to come back after cryotherapy if the tumour is larger than 4cm across. Accordingly it seems patients who benefit from this most are those with a small, early stage kidney cancer who may not be able to have surgery for other health reasons.
Latest studies demonstrate that some drugs may slow the growth of kidney cancer and let patients to live longer. Whereas a complete cure is still a rare occasion, this is still a leap forward. These drugs are taken orally, but they could be related with side effects includes fatigue, hypertension, and also skin rashes. However, for the most part, patients are capable of tolerating these drugs quite well and appear to benefit from them.
Clinical examinations are studies of latest treatments and fresh techniques for treating kidney cancer and other diseases. Taking part in a clinical assessment can offer you a chance to undertake the latest treatments; however it can't guarantee a cure.
Talk about the existing clinical trials with your doctor and cautiously consider the benefits and risks. Several kidney cancer clinical trials are examining innovative and available targeted therapies to settle on the best ways to employ this new class of drugs.
Wednesday, October 29, 2008
Growth hormone replacement in hypopituitarism improves lipid profile and quality of life independently of changes in obesity variables
CLINICAL STUDY
Growth hormone replacement in hypopituitarism improves lipid profile and quality of life independently of changes in obesity variablesPascale Abrams, Hugo Boquete, Hugo Fideleff, Ulla Feldt-Rasmussen, Patrick Wilton, Roger Abs, Maria Koltowska-Haggstrom and Peter Jonsson
P Abrams, endocrinology, university hospital antwerp, antwerp, 2650, Belgium
H Boquete, Hospital T Alvarez, Buenos Aires, Argentina
H Fideleff, Endocrinology Unit, Hospital Municipal T. Alvarez, Buenos Aires, Argentina
U Feldt-Rasmussen, National University Hospital, Copenhagen, Denmark
P Wilton, 7KIGS-KIMS-ACROSTUDY Medical Outcomes, Pfizer endocrine Care, New York, United States
R Abs, Endocrinology, University of Antwerp, Wilrijk, Belgium
M Koltowska-Haggstrom, KIMS Medical Outcomes, Pfizer Endocrine Care, Sollentuna, Sweden
P Jonsson, KIMS Medical Outcomes, Pfizer Endocrine Care, Sollentuna, SwedenCorrespondence: Pascale Abrams, Email: pascale.abrams@belgacom.net
Abstract
Objective: Growth hormone deficiency (GHD) in adults is characterized by elevated body mass index (BMI), increased waist girth (WG) and increased fat mass (FM). Information about how these indicators of obesity affect the lipid profile and quality of life (QoL) of GHD subjects is scarce. It is also unclear how changes in these indicators through GH replacement influence lipids and QoL.
Design and Methods: Adult GHD subjects from the Pfizer International Metabolic Database were grouped according to BMI (n = 291 with BMI <25 kg/m2, n = 372 with BMI 25-30 kg/m2, n = 279 with BMI >30 kg/m2), WG (n = 508 with normal WG, n = 434 with increased WG), and FM (n = 357) and according to changes in these variables after one year of GH replacement. IGF-1 -, lipid concentrations and QoL using QoL-AGHDA questionnaire were assessed at baseline and after one year of treatment.
Results: At baseline, total and LDL-CH were similarly elevated in the BMI and WG groups, but HDL-cholesterol decreased and triglycerides increased with increasing BMI and WG. QoL was progressively poorer with increasing BMI and WG. After 1 year of GH replacement, total and LDL-cholesterol and QoL improved in all BMI, WG, and FM groups.
Conclusions: Variables of obesity adversely affect the unfavourable lipid profile in GHD subjects by decreasing HDL-cholesterol, but do not counteract the positive effect of GH replacement on LDL-cholesterol. Similarly, QoL is influenced by obesity, but responds equally well to GH treatment independent of BMI, WG, and FM.
European Society of Endocrinology http://www.eje.org/cgi/content/abstract/EJE-08-0448v1
Diabetes Insipidus
From http://diabetes.expertinforeview.com/uncategorized/diabetes-insipidus
What is Diabetes Insipidus?
Unlike other types of diabetes such as Diabetes Mellitus Diabetes Insipidus is a disease that is linked to the pituitary gland in the brain. When the word diabetes is mentioned most people will assume that we are speaking of Diabetes Mellitus (Sugar Diabetes). Diabetes Insipidus though is not caused by a lack of insulin or the lack of insulin regulation. Diabetes Insipidus happens when the pituitary gland does not make enough of the hormone ADH. Antidiuretic Hormone is needed to control the amount of water in the body. Diabetes Insipidus can be a serious or even fatal disease if not caught and treated. The treatment may be ongoing for the rest of your life.
What causes Diabetes Insipidus?
Like all forms of diabetes no one knows exactly what causes the actual disease however they do know that people that have had other problems are prime candidates to develop Diabetes Insipidus.
If you have or have had any of the following you may develop Diabetes Insipidus:
* A brain aneurysm which is a weak spot in a blood vessel causing the artery to balloon out much like a weak spot on a tire causes a ?bulge?
* Any type of brain infection
* A Tumor of the brain
* A Tumor of the Pituitary Gland
* Compulsive, excessive fluid intake
* Bleeding inside the skull
* Family history of Diabetes Insipidus
* Head Injury that may cause damage to the Pituitary Gland
* Kidney Disease
* Surgery on the Pituitary Gland sometimes causes a temporary type that lasts about 14 daysIf you have the following signs or symptoms, you should ask your physician to do further testing for possible Diabetes Insipidus:
* Dry skin, especially the hands.
* Constipation
* Passing large amounts of extremely clear urine
* Terrible thirst especially for cold or iced fluidsWhat is the treatment?
The treatment depends more on what appears to be causing the problem. This is one place where the allopathic medical community agrees with the naturopathic medical community. Remove the cause and you treat the disease. This is the underlying theme to most naturopathic treatments, where as the allopathic community is more a symptom treatment practice.
Depending on what may be causing the problem a person may be subjected to any or all of the following tests and or treatments:
> Complete medical history and exam
> Basic Blood and Urine tests
> Computerized Tomography scan (CT Scan)
> Daily weights to determine fluid loss or gain
> Dehydration test
> Intake and output measurements (I and O)
> Magnetic Resonance Imaging (MRI)
> Surgery. If a tumor is involved you may need brain surgery to remove it.Disclaimer:
This report should in no way be considered medical advice. The suggestions and/or techniques described in this report are for informational purposes only. If you are ill or injured you should see your primary healthcare professional immediately
Contact the following groups for more information:
* American Association of Diabetes Educators
American Association of Diabetes Educators
100 West Monroe Street, Suite 400
Chicago, IL 60603-1901
Phone: 1-800-338-3633
Web Address: http://www.aadenet.org* American Diabetes Association
1701 North Beauregard Street
Alexandria, VA 22311
Phone: 1-800-342-2383
Web Address: http://www.diabetes.org* National Diabetes Information Clearinghouse
1 Information Way
Bethesda, MD 20892-3560
Phone: 1-800-860-8747
Web Address: www.diabetes.niddk.nih.govAnnually the American Diabetes Association has a fundraiser bicycle ride called the ?Tour De Cure? I often ride in this event which raises money to help with research to combat diabetes. Be sure to check out my website for details on helping the ADA to find a cure.
Jerry Goodwin has been certified as a Medical Technologist since 1977. He is also certified as a Personal Trainer, Cardiovascular Trainer and Medical exer-therapist. He is a Veteran of the US Navy having served during the Viet Nam era. Jerry also served in the Army National Guard in Ohio, Texas, Kansas and Georgia as a field medic with Infantry, Armored Cavalry, Artillery and Mechanized Infantry Units. He has earned several medals including the Army Commendation Medal. Jerry is the editor of Body Mind and Goals Ezine and the owner of BMG Services Fitness and Nutrition at www.bmgfitness.com
Diagnosis of secondary adrenal insufficiency in patients with hypothalamic-pituitary disease: Comparison between serum and salivary cortisol during the high-dose short synacthen test.
From http://www.eje.org/cgi/content/abstract/EJE-08-0600v1
CLINICAL STUDY
Timo Deutschbein, Nicole Unger, Klaus Mann and Stephan Petersenn
T Deutschbein, Division of Endocrinology, Medical Center, University of Duisburg-Essen, Essen, Germany
N Unger, Division of Endocrinology, Medical Center, University of Duisburg-Essen, Essen, Germany
K Mann, Division of Endocrinology, Medical Center, University of Duisburg-Essen, Essen, Germany
S Petersenn, Division of Endocrinology, Medical Center, University of Duisburg-Essen, Essen, 45122, Germany
Correspondence: Stephan Petersenn, Email: stephan.petersenn@uni-due.de
Abstract
Objective: Accurate assessment of adrenal function is essential in patients with hypothalamic-pituitary-adrenal (HPA) disease. The measurement of salivary cortisol (SaC) instead of serum cortisol (SeC) offers several advantages, such as the determination of the free hormone. We evaluated the diagnostic value of SeC and SaC both unstimulated and during a high-dose short synacthen test (HDT) in comparison to the insulin tolerance test (ITT).
Design: Comparative study between 2005 and 2007.
Methods: Fifty-five patients with HPA impairment and 21 healthy controls were enrolled. Samples were collected in the early morning and over 120 min during the HDT. ROC analysis revealed individual thresholds for four HDT periods (0-30, 0-60, 0-90, and 0-120 min).
Results. The ITT identified 30 subjects as adrenal insufficient. With respect to the four HDT periods, sensitivity and specificity were 67-79% and 71-88% for SeC, compared with 63-72% and 72-86% for SaC. If upper and lower thresholds (with specificities >95%) were applied, patients were diagnosed in 40-45% by SeC, and in 25-31% by SaC. The combination of basal cortisol and HDT allowed a diagnosis in 47-49% (SeC), and in 42%-45% (SaC), respectively.
Conclusion. We suggest the determination of basal SeC or SaC as first-line test. In comparison to the ITT, the HDT has only limited value in screening for alterations of the HPA axis. If the HDT is performed, sampling may be limited to 30 min post-synacthen, using either SeC or SaC. Due to the ease of collection and the independence of binding proteins, SaC may be preferable.
Cushing's Help Newsletter, October 29, 2008
This week's newsletter is here: http://www.mynewsletterbuilder.com/tools/published.php?action=view&newsletter_id=1409748473
In This Issue
What's Happening at the Organization?
New and Updated Helpful Doctors
Book: Disorders of the Human Adrenal Cortex
Endo News: Adrenal Pheochromocytoma
Endo News: Cushing's from Skin Cream?
Endo News: Soroka surgeons removed wrong organ in faulty op
Endo News: Kennedy and Addison's
Endo News: Ask Dr. Gott: Cushing's difficult to diagnose
Doctors on the Move
The Helpful Doctors are moving to their new home. If you are a member Cushie.info, you may add your own Helpful Doctor(s) to the list. As always, advertising is not accepted. Doctors (or doctor's staff members) may not submit his/her own information.
Step by step directions for how to add your Helpful Doctor
• Alabama Doctors
• Arizona Doctors
• Arkansas Doctors
• California Doctors
• Colorado Doctors
• Connecticut Doctors
• Florida Doctors
• Georgia Doctors
• Idaho Doctors
• Illinois Doctors
• Indiana Doctors
• Kansas Doctors
• Kentucky Doctors
• Maine Doctors
• Massachusetts Doctors
• Maryland Doctors
• Minnesota Doctors
• Missouri Doctors
• Nebraska Doctors
• New Jersey Doctors
• New Mexico Doctors
• New York Doctors
• North Carolina Doctors
• Ohio Doctors
• Oklahoma Doctors
• Oregon Doctors
• Philadelphia Doctors
• South Carolina Doctors
• Tennessee Doctors
• Utah Doctors
• Virginia Doctors
• Washington Doctors
• Washington, DC Doctors
• Wisconsin Doctors
• Puerto Rico Doctors
• UK Doctors
Monday, October 27, 2008
Endocrinology
From http://lifeasamedicalstudent.blogspot.com/2008/10/endocrinology.html
Hormonal regulation is much more complex than I first imagined, but it is incredibly interesting too.
Endocrine System
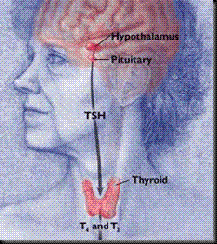
Our recent studies have initiated investigations into the complex world of glands and their secretions.Complemented by histological examinations of cellular breakdown, endocrine physiology, too, has been presented for study. Our first stop was the pituitary followed by the thyroid.
The endocrine glands regulate bodily functions trying to keep us in a healthy state. When secretions become too low or too high, normal functions are compromised and disease ensues. The thyroid in particular has me quite fascinated, perhaps due to recency.
Thyroid
This butterfly like gland found just below our voice box controls many functions and is most commonly known to have an effect on our body's metabolism. It requires a minimal level of iodine from our diets which can be found in many water sources, salt, meat, fish and vegetables. In cases of hyperthyroidism (too much hormone) individuals commonly lose weight and have tissue swelling. The opposite, hypothyroidism, causes weight gain and can lead to the growth of thyroid tissue also known as a goiter. As with every other part of the body, thyroid cancer can have deleterious effects similar to those mentioned above.
These are only some of the effects of thyroid hormones and many others are integrated with various body systems. My first thought was why not give low doses of thyroid hormone to help people lose weight. It sounds like a rather easy solution until you start to factor in all the other problems that would arise from altering the normal hormonal levels. Needless to say, I am still a neophyte when it comes to all of this, but for the moment it piques my interest.
Friday, October 24, 2008
Answering Your Autoimmune Diseases Questions
From http://www.content4reprint.com/health/answering-your-autoimmune-diseases-questions.htm
In health class you are taught about how the body has its own defense mechanism called the immune system. In a healthy body the immune system works to keep out infection and keep the body from developing colds, flues, and other diseases. It works around the clock to protect the body from outside intruders. But what happens when the immune system does not work as it should? It stops protecting the body and instead begins to attack it.
That is what autoimmune diseases are. Autoimmune diseases are when the body begins to attack its own tissues and organs. This can prove quite problematic for the host body and over time without the proper care it can cause the person to become gravely ill or even die.
It is not an easy condition to have and it is one that must be constantly monitored at all times. In this article we will discuss autoimmune diseases and how they can affect you and your body.
What are some examples of autoimmune diseases?
There are many, many autoimmune diseases to choose from. They range from Acute disseminated encephalomyelitis to, Graves' disease, Narcolepsy to Wegener 's granulomatosis. Each disease is different in how it manifests itself. There are some diseases such as Schizophrenia that many people do not realize is an autoimmune disease.
These are serious diseases that have caused misery to those that have them. But each day more and more research is done to understand why these diseases develop and if there is a cure that can be found or manufactured.
But until that time most patients have to live with the disease and its effects on their daily lives. It is not an easy life and it is one filled with numerous trips to various doctors.
What are the symptoms for some autoimmune diseases?
Autoimmune diseases differ widely by each disease. There are many symptoms that can seem alike but are in actuality different diseases. In Addison 's disease it is a rare endocrine disorder where the adrenal gland does not produce the necessary hormones needed for the body to survive. The symptoms of Addison 's disease can be commonly mistaken for other illnesses.
Common symptoms of Addison 's disease are muscle weakness, fatigue, weight loss, changes to the person 's mood and personality along with a host of other symptoms. Each of the symptoms by itself is nothing remarkable and can be explained away as a common cold or the flu. But when physicians begin looking at the total symptoms presented along with performing endocrine tests, and then the likelihood for a diagnosis of Addison 's disease becomes present.
What are some tips for dealing with these diseases?
The best tip for dealing with autoimmune diseases is to lead a healthy life. This means eating a balanced diet rich in fresh vegetables and fruits. It also means exercising daily to help the body stay strong and active. You can also lessen the impact of the disease on your life by learning how to meditate to take your mind off your aches and pains.
You should also get plenty of rest. Some nights this may seem impossible when the disease is active but you can get sleeping medication and better sleeping methods from your doctor. It may also help to talk to a therapist about your disease and how you can take the strains and pressures of work and life off your shoulders. You must keep your body healthy and that includes keeping your mind healthy as well.
Can I lead a normal life while dealing with autoimmune diseases?
Yes, you can lead a normal life when dealing with autoimmune diseases. It will take some effort and work on your part but you can live as you used to before the diagnosis. The key is to learn to work around your disabilities.
By keeping your body and mind healthy you can work through any problems that present themselves. You are the most important factor in living a healthy, normal life. Will it always be easy? No, but few things are easy. Many people live with their conditions everyday and do not let the disease live their lives for them. You can do the same too.
Disorders of the Human Adrenal Cortex
Disorders of the Human Adrenal Cortex (Endocrine Development,)
By C. E. Fluck, W. L. Miller
* Publisher: S. Karger AG (Switzerland)
* Number Of Pages: 164
* Publication Date: 2008-07-15
* ISBN-10 / ASIN: 3805585802
Product Description:
Substantial further advances in our understanding of adrenal development, steroid biosynthesis and adrenocortical disorders necessitate another look at this small but complex organ. In this volume, leaders in the fields of adrenal development, biochemistry and genetics review the most recent findings from bench and bedside research. New aspects of adrenal development and zonation and the novel >backdoor' pathway to androgen synthesis are discussed. P450 oxidoreductase deficiency (a newly described form of congenital adrenal hyperplasia) and long-term outcome of prenatal treatment of 21-hydroxylase deficiency are examined.
An update on ACTH resistance and adrenal Cushing's syndrome is provided. Finally, the role of adrenal steroidogenesis in arterial hypertension and fetal programming of adrenal androgen excess as a possible explanation for polycystic ovary syndrome in later life are analyzed.
This book will be of great interest to pediatric, adult and reproductive endocrinologists, clinical geneticists, developmental biologists and basic scientists working in the fields of endocrinology and steroidogenesis.
PDF | 1.7 MB
http://w13.easy-share.com/1702124224.html
or
http://www.share-online.biz/download.php?id=1D36E89F16
or
http://uploaded.to/?id=3lkqa0
or
http://www.megaupload.com/?d=KKY70OB4
Thursday, October 23, 2008
Cushing's From Skin Cream?
From http://www.cbn.com/CBNnews/469012.aspx
China's golden Olympic media glow has definitely worn off, largely due to the melamine-laced baby formula. Unfortunately, milk-based products aren't the only Chinese items to have soured. Over the past few weeks, several others, ranging from baby cribs to beans to dog food, and even Chinese medicines.
.....
Skin Cream: One Chinese skin cream was banned after officials found it contained a steroid hormone called clobetasol propionate. While the hormone can be used to treat skin disorders, it can also cause changes in blood sugar, abnormal growth of body and facial hair, emotional disorders, and Cushing's syndrome.
One eight-month old girl allegedly began to menstruate after using the cream for seven months, and her mother wouldn't have known that the cream contained the hormone, since the package did not even mention the hormone. Instead, it said it was only composed of all-natural ingredients.
......
Follow Up here: http://www.straitstimes.com/Breaking%2BNews/Asia/Story/STIStory_293598.html
Chinese skin cream recalled
An 8-month-old girl had appeared to menstruate after being given the cream for seven months.
BEIJING - A COMPANY in south-west China has recalled a skin cream after a potentially dangerous steroid hormone that should not be used for more than two weeks was found in it, state media said on Wednesday.
The Miaoling Medical Technology Group, based in Guizhou province, also said it had stopped production and sales of the cream, which was widely used to treat eczema in babies, the Beijing Youth Daily reported.
The hormone - clobetasol propionate - used to treat various skin disorders, should not be used by children under 12, according to drug information website drugs.com.
It can cause changes in blood sugar and can lead to Cushing's syndrome, a disorder characterised by a moon-shaped face, emotional disturbances, and in women, abnormal growth of facial and body hair.
The packaging of the cream, however, claimed it consisted only of 25 natural ingredients, according to an earlier report on Guangzhou news website gznet.com.
A report in Xiaoxiang Morning News in central China said that an eight-month-old girl in Changsha, the capital of Hunan province, had appeared to menstruate after being given the cream for seven months.
Doctors said they suspected the hormone was the cause, the paper said.
Another report published on the popular web portal sina.com said Guizhou's health department had fined the company 5,000 yuan (about $1,100) as far back as August 14 when it discovered the hormone in a test of the cream.
The report, citing a local paper in east China, said the product's license was in the process of being revoked.
The news comes as China is still reeling from a tainted milk scandal that has led to recalls and bans of Chinese-made dairy products around the world.
Milk made by 22 Chinese dairy companies was found to have been contaminated wth melamine, an industrial chemical normally used to make plastic, causing the death of at least four babies and sickening another 53,000.
Calls made to the skin cream company and to the Guizhou health department went unanswered on Wednesday. -- AFP
Monday, October 20, 2008
Soroka surgeons removed wrong organ in faulty op
From http://www.haaretz.com/hasen/spages/1029926.html
By Ran Reznick
Surgeons at Soroka Medical Center in Be'er Sheva earlier this year erroneously removed part of a patient's pancreas instead of his adrenal gland, which is located above the kidneys. They later discovered the operation had been based on a faulty diagnosis and had been unnecessary from the start, Haaretz has learned. The patient suffers from Cushing's syndrome, an endocrine disorder caused by high levels of cortisol in the blood.
After the operation, the man was admitted to intensive care, where he became stricken with diabetes. He has since received daily insulin injections, the dosage of which he says continues to increase on a daily basis. As a result of the mishap, the patient's pancreas became infected and the 32-year-old Be'er Sheva man had to undergo a second operation.
Last week, seven months after undergoing the wrong procedure in March, he underwent the brain procedure he should have originally undergone at Tel Aviv's Assouta Medical Center. During that procedure, it became clear the root of the man's medical problems indeed lay in the pituitary gland in the brain.
The faulty operation was carried out on March 30 at Soroka, and Haaretz obtained the details surrounding it from a team of senior physicians at Soroka and Maccabi.
An investigation into the matter revealed that the Soroka management, led by Dr. Michael Sherf, never reported the unusual incident to the Health Ministry.
Failed to report
The procedure was carried out by a surgical team led by Prof. Salim Suli Mizrahi, Dr. Eliezer Avinach and Dr. Abd al-Rahman Abu Ghanim. The hospital told Haaretz that it did not report the matter because the incident did not represent the "erroneous removal of an organ," which ministry regulations demand be reported, but rather the partial removal of part of an organ.
A senior health system official told Haaretz that Soroka management was required to report the incident to the ministry, and that the incident called for a thorough investigation by an investigative committee to examine the conduct of the physicians involved in the faulty procedure.
The hospital management did report the incident, however, to the insurance company that handles malpractice lawsuits against physicians.
A senior surgeon who looked into the incident said, "the operation should not have been carried out until the medical examination was complete. There is a chain of mistakes here which apparently stems from a lack of sufficient experience among surgeons to carry out such procedures, or from a lack of caution in doing the operation."
"The pancreas is located next to the adrenal gland, and here the surgeon's experience should come into play, and he should identify the organ and not cut into another one close to it. The suspicion of a mistake should have come up in the operating room, due to the size of the organ that was removed," he added.
A senior internal medicine specialist said he also believed the operation should only have been conducted after a comprehensive check of the man's medical problems.
"This was poor medicine, and there is a basic, systemic medical failure which includes the way in which the patient was transferred from the HMO to the hospital. This is a serious incident that led to unnecessary surgery, which endangered the patient's life and the outbreak of severe diabetes," the official said. "The incident demands a thorough investigation, arriving at systemic conclusions and a personal examination of responsibility of the physicians involved at both Soroka and Maccabi."
Two days after the erroneous operation, the patient was examined by Prof. Yair Liel, the head of Soroka's endocrinology unit. Liel determined that in contrast to the initial diagnosis, the patient's medical problems had their roots in the brain. He also recommended that the man be referred to Dr. Jonathan Arbel, the head of endocrinology in the HMO's Negev district.
The patient underwent the second, correct surgery on his brain last Thursday. His family told Haaretz the procedure was carried out successfully, and was able to determine the root of the man's symptoms.
A response from Soroka Medical Center said the hospital "has successfully carried out dozens of laparoscopic surgeries to remove the adrenal gland, the majority by Prof. Suli Mizrahi and Dr. Eliezer Avinach, senior surgeons with vast experience in the field."
"Placing a report with the Health Ministry is required when dealing with the removal of an essential organ in an erroneous manner," said spokeswoman Inbar Darom-Gutter. "The portion of tissue removed was marginal, and does not affect the function of the pancreas or influence its operation."
Maccabi HMO spokesman Ido Hadari said "this is an unfortunate incident and we hope the patient's condition improves soon. Maccabi operates in a transparent manner with the Health Ministry and reports every incident required by law."
Sunday, October 19, 2008
Kennedy and Addison's Disease
From http://www.washingtonpost.com/wp-dyn/content/article/2008/10/17/AR2008101702058_pf.html
 The picture of health: Back pain forced President Kennedy to use an Air Force lift to board his plane. Voters never knew the extent of his ailments. (AP Photo/Harold Valentine)
The picture of health: Back pain forced President Kennedy to use an Air Force lift to board his plane. Voters never knew the extent of his ailments. (AP Photo/Harold Valentine)
A Hale Chief? Better Check Up on That.
By Robert Dallek
Sunday, October 19, 2008; B03
The American public seems pretty sure that it knows everything it needs to know about whether John McCain and Barack Obama are healthy enough to be president. I'm not. And whenever I think about whether both men are fit to serve, physically speaking, I think about the sinking feeling I had one lovely spring afternoon in 2002 when an archivist at the John F. Kennedy Presidential Library wheeled out the cartload of files showing how badly we had all been deceived about JFK's health.
The secret details of Kennedy's medical history were buried in 10 beat-up old cartons of records the library had held for 40 years. Past requests for access to these materials had all been refused by a committee of loyalists that included one of JFK's closest advisers, speechwriter Ted Sorensen. To my surprise, the committee had given me the chance to read the files; I had to agree not to photocopy them but was free to take notes or read passages into a tape recorder. Now I -- along with a physician friend, Jeffrey Kelman -- felt as if I were breaching a wall of secrecy. Here were not the usual neat boxes of presidential records, preserved in red-blue-and-silver-trimmed containers, but musty cardboard cartons that seemed to have sat untouched in some corner of the library since Janet Travell, one of Kennedy's physicians, had given them to the library after JFK's assassination in November 1963.
Between May 1955 and October 1957, Kennedy had been hospitalized nine times for a total of 44 days, including one 19-day period and two week-long stretches. Despite his public image of "vigah," as his accent rendered it, he suffered from bouts of colitis, accompanied by abdominal pain, diarrhea and dehydration; agony in his back triggered by osteoporosis of the lumbar spine; prostatitis, marked by severe pain and urinary infections; and Addison's disease, a form of adrenal insufficiency. Some of his difficulties, such as his back pain and Addison's, were open secrets among the press corps during his 1960 run for the White House, but the extent and severity of his problems -- to say nothing of the promiscuous variety of medications and doctors he relied upon to maintain his health -- had remained undisclosed. That's largely because the Kennedy campaign made every effort to hide his health problems -- obviously convinced that these disclosures, combined with his youth and Catholicism, would sink him.
Kennedy was following in a little-known but troubling tradition in American politics -- and one we should remember when we assume that McCain and Obama have told us everything we need to know. Since that day at the Kennedy library, I have been advocating the full disclosure of all presidential candidates' medical histories, physical and psychological, in no small measure because the Kennedy campaign's deceptions were in line with the deceits or shadings offered by Woodrow Wilson and Franklin D. Roosevelt during their own presidential bids.
Unbeknownst to the public, Wilson had suffered several small strokes before he ran in 1912 and continued to suffer them while in office; they proved to be preludes to a massive stroke in September 1919 that left him with a paralyzed left arm and leg and limited cognitive function. He could not stay alert for sustained periods of time or keep anything resembling a normal presidential work schedule. But the White House hid, as best it could, the extent of the president's incapacity from the public. Even though Wilson still had 18 months remaining in his term, which was being dominated by an economic recession and widespread fears of radicalism provoked by the Bolshevik revolution in Russia, the press, foolishly, deferred to the president's desire for privacy. White House subordinates declined to reveal the truth about the president's condition -- an amazing display of recklessness.
The public did not fully understand how badly Roosevelt's health was failing when he ran for a fourth term in 1944. He died the following April, during the waning months of World War II, of a cerebral hemorrhage brought on by arteriosclerosis. When Winston Churchill's physician saw FDR at Yalta in February 1945, the British doctor predicted that the president would be dead in a matter of months. After his death, shocked Americans wondered whether he should have run again in 1944 and whether he had performed as effectively as he might have at the Yalta conference with Stalin.
If Wilson, Roosevelt and Kennedy had fully disclosed their health problems, it might have cost them the Oval Office. Wilson would have been pressured to resign, something he considered doing in January 1920, and turn the presidency over to his vice president, former Indiana governor Thomas R. Marshall. Wilson's and his closest advisers' decision to keep the president's disability secret was an undemocratic abuse of presidential power.
If FDR and JFK had allowed the public to know about their own health problems in 1944 and 1960, respectively, they might well have lost. Then again, Roosevelt's hold over the electorate remained considerable, so he might have prevailed. And if JFK had leveled with the public about the pain he bore, he might have been seen as heroic for achieving so much despite his suffering.
But such calculations are beside the point, then and now. Politicians' political problems are their own. Their health problems belong to all of us, and if candidates don't like that, they need not run for president. It was and is the public's right to have the fullest possible information about a potential president's physical condition. If you want to be the most powerful person in the world, you will also have to be one of the least private. Voters deserve to know the full picture -- no ifs, ands or buts.
Those who squirm at this standard often point to the examples of Abraham Lincoln and Winston Churchill, both of whom suffered from depression, and argue that these titans might never have taken office if they had offered full disclosure of their emotional struggles. I do not take so dim a view of the electorate and believe that American and British voters would still have recognized their greatness. Democracy rests on informed decision-making, and I see no decent argument for secrecy -- especially if we may be passing the world's largest nuclear arsenal into ailing hands.
So on Oct. 3, when I read a full-page ad in the New York Times by 2,768 medical doctors calling on John McCain to release fully his health records to the public, I cheered. The voters' judgments should rest on the fullest possible information about the presidential candidates' potential performance in office. The fact that McCain could be our oldest elected president, a 72-year-old man with a history of skin cancer and a largely untested running mate, makes it all the more urgent that we know more about his health before voting. It's admirable that he shared 1,173 pages of his medical records with a small number of reporters during a three-hour period in May. But the limits the McCain campaign imposed on the review of those materials -- the eyebrow-raising time constraints, the exclusion of a New York Times reporter with an M.D. from the pool, the refusal to permit photocopying -- raise questions about what medical experts might find if given unrestricted access.
The requirement for full disclosure should apply to Barack Obama as well. His campaign has released only a single page of information about his health history. He is just 47 and seemingly in excellent health, but nobody is immune from illnesses that voters might want to take account of in November. And remember, we all thought JFK was the picture of youthful vigor, too.
Advances in modern medicine and in public understanding of diseases suggest that someone with a history of cancer or some other life-threatening illness need not be seen as barred from serving as president. But in an era when presidents shoulder such staggering responsibilities, voters in the United States -- and people around the world -- are entitled to know as much as possible about the person who will have so much to say about all our lives and futures.
Robert Dallek is the author of "An Unfinished Life: John F. Kennedy, 1917-1963." His latest book is "Harry S. Truman."
Saturday, October 18, 2008
Follow-up to yesterday 2
Well, the energy from the Adrafinil is a one day thing. I felt great on Thursday. Friday and Saturday I slept more than usual. Saturday, today, was one of those days where I sleep nearly all day. Maybe if I took the drug more it would build up in my system, maybe not. But it was still worth having that one day where I felt what I imagine normal to be.
While I was being a slug today, my husband painted the entire house.
I'm not sure if I would have been this tired today or if I was somehow making up for the nap I didn't get on Thursday. Whatever the case, I'm glad that I had the opportunity to try this and to experience the wonderful effects, if only for one day.
Information from a site that sells this:
Alertness Without Stimulation
Adrafinil is the prototype of a new class of smart drug - the eugeroics (ie, "good arousal") designed to promote vigilance and alertness. Developed by the French pharmaceutical company Lafon Laboratories, adrafinil (brand name, Olmifon) has been approved in many European countries for treating narcolepsy, a condition characterized by excessive daytime sleepiness and other unusual symptoms.
Non-narcoleptic users generally find that adrafinil gives them increased energy and reduces fatigue, while improving cognitive function, mental focus, concentration, and memory. It has been reported that quiet people who take adrafinil become more talkative, reserved people become more open, and passive people become more active.
Of course, many stimulant drugs, ranging from caffeine to methamphetamine, are known to produce similar alerting/energizing effects. Adrafinil has been described by some users as a "kinder, gentler" stimulant, because it provides these benefits but usually with much less of the anxiety, agitation, insomnia, associated with conventional stimulants.
Adrafinil's effects are more subtle than those of the stimulants you may be used to, building over a period of days to months. They appear to be based on its ability to selectively stimulate 1-adrenergic receptors in the brain.2 These receptors normally respond to norepinephrine (noradrenaline), a neurotransmitter linked to alertness, learning, and memory. This is in contrast to conventional stimulants, which stimulate a broader spectrum of brain receptors, including those involving dopamine. Its more focused activity profile may account for adrafinil's relative lack of adverse side effects.
There's more info about Adrafinil on Wikipedia
It's interesting that that snipped report that people become more talkative. I reported that in the original post, too, even though I didn't realize that this was a possibility.
A good quote that I wish I could relate to better:
"Time is limited, so I better wake up every morning fresh and know that I have just one chance to live this particular day right, and to string my days together into a life of action and purpose."
Lance Armstrong (1971 – )
Cyclist, seven-time Tour de France champion and cancer survivor
Friday, October 17, 2008
A Completely Different "Yesterday" Post
Wow. That's about all I can say. Yesterday was possibly the best day of my life since I started getting Cushing's symptoms, and that was over 25 years ago. A quarter of a century of feeling exhausted, fatigued. A quarter of my life spent taking naps and sleeping.
Last week in this post I wrote in part:
I went to the endo yesterday. Nothing has changed for me. Nothing will. He wants me to take more cortef. I don't want to gain weight again. He looked up Provigil and it's not indicated for panhypopituitarism. So he won't prescribe it. My kidney surgeon probably won't let me take, anyway, but it was worth a try.
...
He did mention that in "only" 2.5 years maybe I can go back on growth hormone. I don't want to live like this another year let alone 2.5. But then, when I was on GH before it didn't help me like it helps most everyone else.
I'm tired of catering to a kidney that may or may not fail sometime anyway, tired of being so exhausted all the time. I feel like I've lost nearly half my life to this Cushing's stuff already.
So, yesterday I was supposed to go to a conference on web design for churches. My church sent me because they want me to spiff up their site and make them a new one for Christmas. I wanted to go because, well, I like learning new stuff about the web. I figured that I would learn stuff that would also be useful to me in others of my sites.
And I did!
But the amazing thing is this. My son had told me about a medication that was very similar to Provigil, that he had tried it while he was writing his doctoral thesis and it had helped him.
So, having tried the official doctor route and being rebuffed - again - I had decided to try this stuff on my own.
Just the night before I had written a response on Robin's wonderful blog that reads in part:
I hate this disease, too.
I was just talking to a friend today about how I'd try nearly anything - even if it ruined my one remaining kidney - to have a few days where I felt good, normal, where I could wake up in the morning rested and be able to have energy for the day.
I want to go out and have fun, to be able to drive for more than 45 minutes without needing to rest, to be have people over for dinner, whatever. I hate being restricted by my lack of energy.
My endo says to cheer up. In two and a half years I can try the growth hormone again. Whoopee. Didn't work the first time and maybe gave me, or contributed to, cancer growth. Why would I want to look forward to trying that again?
I want to feel good now. Today.
I hate that this disease kills but I also hate that it's robbed me of half my life already.
I wish doctors would understand that even though we've "survived", there's no quality of life there.
I hate Cushing's. It robs so much from so many of us. :(
As I said earlier, I have a history of daily naps of at least 3 hours a day. It cuts into everything and prevents me from doing many things. I have to schedule my life around these naps and it's awful.
 A few years ago I went on a Cushie trip to Rockford. I've been there a few times and it's always so much fun. But this first year, we were going to another Cushie's home for barbecue. I didn't drive, I rested in the back of the car during the drive. We got there and I managed to stay awake for a little while. Them I put my head down on the dining room table and fell asleep. Our hostess kindly suggested that I move over to the sofa.
A few years ago I went on a Cushie trip to Rockford. I've been there a few times and it's always so much fun. But this first year, we were going to another Cushie's home for barbecue. I didn't drive, I rested in the back of the car during the drive. We got there and I managed to stay awake for a little while. Them I put my head down on the dining room table and fell asleep. Our hostess kindly suggested that I move over to the sofa.
So, I have a long history of daily naps, not getting through the day, yadda, yadda.
So, I was a little nervous about yesterday. I really wanted to go to this conference, and was afraid I'd have to go nap in my car.
I got up at 5:30 am yesterday. Before I left at 7:15, I took my Cortef and then I took my non-FDA approved simulated Provigil. (Although it's not FDA approved, it is not illegal to possess without a prescription and can be imported privately by citizens)
I stayed awake for the whole conference, went to a bell rehearsal, did Stacey's interview, had dinner and went to bed about 10:30PM. NO NAP! I did close my eyes a little during the 4:00PM session but it was also b-o-r-i-n-g.
I stayed awake, I enjoyed myself, I learned stuff, I participated in conversations (completely unlike shy me!).
I felt like I think normal people feel. I was amazed. Half my life wasted and I finally (thank you Michael!) had a good day.
My kidney doctor and my endo would probably be appalled but it's about time that I had some life again! Maybe in another 25 years, I'll take another pill. LOL
Tuesday, October 14, 2008
Drat!
Another Cushing's patient has died :( Over the years that I've been running the Cushing's sites, we have lost at least 16 Cushies - about 2 a year - that I know of. I wonder how many others there have been that I don't know about. Or they weren't even diagnosed yet at the time that they died.
Somehow, we have to get the system improved, to save the lives of more Cushies, known and unknown to us.
Even before I heard of the Internet, while I was waiting for surgery at NIH, a woman with Cushing's died. I would not have known except that there was an article about her in my college alumni magazine. She had been my age, lived in my city, graduated from my college with my major the same year as I did, was also a teacher, had my doctor... It could have been me. Thank goodness I didn't read about that until after my surgery.
The patients I have known about who died - 3 I have known very well. We had gotten to be good friends over the years. We managed to share good times, laughs, times of thoughtfulness, times of sadness, many phone calls and visits, adoptions of children, births of grandchildren, even a vacation! Just like "normal" friends. But we were bound by the bonds of Cushing's and we understood each other.
Even though I didn't know Martha who died last night, her death saddens me deeply. Too many deaths, too young.
Someday, I'd love to meet a Cushie in her 90's or older!
Sunday, October 12, 2008
Neuroimaging of pituitary adenomas
The author: Professor Yasser Metwally
INTRODUCTION
October 11, 2008 — In this edition of the monthly publication “Topic of the month” Professor Metwally discusses the neuroimaging findings in pituitary adenomas. This topic is presented in downloadable PDF format.
Click here to download this monthly topic (Neuroimaging of pituitary adenomas) in PDF format (570 KB)
Originally termed chromophobe adenomas, endocrine-inactive pituitary tumors were once considered the largest group of pituitary tumors. With advances in endocrinologic testing and modern immunohistochemical and immunoelectron microscope techniques, the incidence of adenomas with no evidence of hypersecretion or endocrine activity has decreased to about 25 per cent of pituitary adenomas. Histologically, these adenomas have secretory granules and immunocytochemically are growth hormone or prolactin-positive, despite no associated clinical changes or abnormal serum hormone levels about 5 per cent of the time. Inactive tumors have cells with no histologic, immunocytologic, or electron microscopic markers (Null cells). They are chromophobic and electron microscopy show them to have poorly developed cytoplasm, indented nuclei, and sparse granules (100 to 250 lim) lined up along the cell membrane.
It is the functionally active group of pituitary tumors that comprise the largest percentage of pituitary adenomas. They represent about 75 per cent of all pituitary tumors. Preoperative endocrinologic testing, as well as clinical symptomatology resulting from the adenoma’s hypersecretion of hormones, helps to identify and classify these tumors. It is this functional classification confirmed with immunohistochemical and immunoelectromicroscopic techniques and not traditional light microscopic pathology that separates these tumors.
Prolactinomas represent about 40 to 50 per cent of all patients with pituitary adenomas. Under light microscopy, prolactin cell tumors are chromophobic or acidophilic. Using immunoelectron microscopy, they may be classified as densely or sparsely granular, although the former type is quite rare. The densely granular resemble nontumor lactotrophic pituitary cells that are resting and nonsecreting. The sparsely granular type resemble the nontumor lactotrophic pituitary cells that are actively secreting. Their secretary granules are sparse, spherical, and measure 150 to 350 nm.
Somototrophic adenomas, resulting in acromegaly, account for 15 to 25 per cent of pituitary adenomas. Under light microscopy, these tumors may be termed acidophilic or chromophobic. Using immunoelectron microscopy, two distinct cell types can be identified: densely and sparsely granulated adenomas. The densely granulated cell type more closely resembles nontumor pituitary somototrophic cells and is characterized by well-developed endoplasmic reticulum, permanent Golgi complexes, and numerous spherical densely staining secretary granules. The sparsely granulated type differ from nontumorous pituitary somototrophic cells in that it has permanent Golgi complexes, irregular nuclei, few spherical secretary granules, and several centrioles.
Cushing’s disease or Nelson’s syndrome caused by corticotropin-secreting adenomas represent only about 5 per cent of all pituitary adenomas. Under light microscopy, corticotrophs are basophilic. Immunoelectron microscopy shows these tumor cells to be similar to corticotrophic nontumorous pituitary cell types containing numerous spherical secreting granules that vary in density, measure 250 to 700 nm, and line up along the cell membranes.
The rarest of pituitary adenomas are those that secrete solely thryotrophin or gonadotropin. Each type accounts for less than 1 per cent of pituitary adenomas. Under light microscopy, the thyrotropic adenomas are chromophobic and under electron microscopy, they have long cytoplasmic processes, sparse, spherical secreting granules (150 to 250 nm), and abundant endoplasmic reticulum.
Pituitary macroadenomas are, by definition, at least 10 mm in size or more, while microadenomas are less than 10 mm in size.
Click here to download this monthly topic (Neuroimaging of pituitary adenomas) in PDF format (570 KB)
References
Metwally, MYM: Textbook of neuroimaging, A CD-ROM publication, (Metwally, MYM editor) WEB-CD agency for electronic publication, version 9.4a October 2008 [Click to have a look at the home page]
Saturday, October 11, 2008
Elvis as Cushie?
from http://wehasspoken.blogspot.com/2008/10/elvis.html
Elvis
I don't think you can get more on fire than the late Elvis Presley. I spent this morning reviewing youtube clips of his last few concerts. He is not just fat, he has the look of someone with Cushing's syndrome. This is a condition where there is elevated cortisol in the blood stream creating edema in the extremities and the characteristic "moon face." It is more than the look of someone who had too many pancakes and beer....
"Kidney Cancer is NOT a death sentence" says broadcaster James Whale
From http://maturetimes.co.uk/node/6708
By Jayne Warren - 10/10/2008
Every year almost 6,200 people in the UK learn that they have kidney cancer - more than are killed in road accidents - yet the condition rarely attracts much public attention or funding for research. Even worse, the proven drug treatment, Sutent, is not licenced by NICE, so sufferers are subject to the dreaded 'PCT' lottery. But James Whale, who was diagnosed with "a tumour the size of a football" in 2000 and subsequently founded the James Whale Fund for Kidney Cancer, is on a mission to change all this...
"Frankly, I'm really angry about NICE's refusal to licence Sutent. Really angry about it - especially as it has been thoroughly tested and significantly improves the lives of those with advanced kidney cancer. NICE claim they are 'protecting us', but in my view what they are doing is evil," said James in his famously rich, warm voice. Renowned for talking straight, he certainly doesn't mince his words about a subject that is so dear to his heart.
"The problem with kidney cancer is that there are very few symptoms. Feeling a bit tired, perhaps, not much appetite, night sweats - could be loads of things. I'd just got back from holiday and felt really great, but found I had blood in my urine. Didn't really bother me much. And despite my wife's pleas, I didn't bother to visit the doctor."Eventually I took a one-off test in a centre at Waterloo Station, which led to me seeing my own doctor for more tests, and ended up with my brilliant specialist surgeon, Tim O'Brien, informing me that I had the biggest tumour he'd ever seen," said James. "Thank God I hadn't cancelled my health insurance! It was a primary cancer, hadn't spread and looked like a mushroom pizza - but the biggest problem was how to get the thing out!"
James was booked in for surgery within a few days, taking the precaution of spending the weekend before in Brighton with his wife "getting paralytic". They both had to face the fact that it might be their last few days together.
Fortunately for them, for thousands of radio listeners and now kidney cancer sufferers, the operation went well. "They had to cut me in half to get it out, so I've got a scar from under my arm right down to my groin. Massive," said James blithely, who has remained cancer free, lives without one kidney - and takes no medication at all.
Unsurprisingly, the experience made him realise just how little help and advice there was for kidney cancer patients, to say nothing of the appalling availability of Sutent across the UK's PCTs. In true James Whale style, he decided to do something about it, and since then has become a very vocal advocate for sufferers. The James Whale Fund for Kidney Cancer supports research into the causes, prevention and treatment of the disease, and provides a support network offering advice, information and encouragement to those who’ve been diagnosed with kidney cancer and their carers.It also acts as a campaigning arm to get Suten licenced by NICE. "NICE have got loads of money, loads, but they stand by and do nothing while lives are being lost. They claim that Suten is too expensive, but the real reason they are expensive is because the drug companies bear the costs of developing the drug and the licence" he said, his voice thick with years of genuine frustration.
"So why don't NICE grant a long licence, so the drug can be copied and then made available to everyone at a much lower cost? They're funded by the Government. But why don't the drug companies and the Government work together to sort licences out in the first place, rather than spending millions on NICE?
"I'm angry because the drugs ARE there, they ARE available, they CAN be prescribed - but they are being blocked. My worry is that with the inconsistent relationships between PCTs across the UK, all that will happen is GPs will find more sufferers of kidney cancer - and not be able to give them the drugs they need to either save or lengthen their lives.
"2008 must be the year that marks kidney cancer as the awful disease it is, and sees the PCTs, NICE and GPs working to the common goal of reducing the harm caused by the disease. I just hope that the new system being considered whereby patients can pay for their own drugs whilst being treated in an NHS setting will make a big difference. Its not ideal, but it will save lives - and that's what matters."
James is quite open about accepting money "from wherever he can" to help keep his Fund afloat and thereby help others. "I just keep asking for donations. I'm not proud. My message to anyone reading this is simple: I want people to realise that cancer is NOT a death sentence. If you catch it early enough, it's treatable. I HAD cancer - not any more."So why the UK Curry Party from October 19th-25th?
"I like curry."So what's going on? Restaurants and homes across the UK are signing up to hold a Curry Party over the week of 20th October in support of James' charity for Kidney Cancer. Launching at the British Curry Awards at The Grosvenor House Hotel on Sunday 19th October, the following week will be crammed with public and private curry events across the UK.
The idea is not just to raise funds but also awareness of the disease and potential treatments.
Parties can be planned at home or in public using recipes and party ideas available in ‘host party packs.' Funds are raised from donations made by friends and family who attend, and all money raised is paid directly into the Fund's bank account. Big public events are planned for London (20th), Manchester (21st) and Thursday 23rd is set aside for ‘at home’ or 'corporate curry party'. Friday 24th is the culmination of ‘Britain’s Biggest Curry Party' in London, with an evening hosted by James Whale and renowned TV chef Cyrus Todiwala MBE.
Friday, October 10, 2008
Yesterday
No, it's not just a Beatles song.
I went to the endo yesterday. Nothing has changed for me. Nothing will. He wants me to take more cortef. I don't want to gain weight again. He looked up Provigil and it's not indicated for panhypopituitarism. So he won't prescribe it. My kidney surgeon probably won't let me take, anyway, but it was worth a try.
He did take more blood than usual. One tube was ACTH, another renin. I don't know what the other tube was for. Probably just general metabolic.
I don't think I've ever had renin levels tested before. When I looked that up, there's a lot of kidney stuff. I sure hope that there's nothing wrong with my kidney. I've been so careful.
He did mention that in "only" 2.5 years maybe I can go back on growth hormone. I don't want to live like this another year let alone 2.5. But then, when I was on GH before it didn't help me like it helps most everyone else.
I'm tired of catering to a kidney that may or may not fail sometime anyway, tired of being so exhausted all the time. I feel like I've lost nearly half my life to this Cushing's stuff already.
A bit about rennin levels from http://www.healthatoz.com/healthatoz/Atoz/common/standard/transform.jsp?requestURI=/healthatoz/Atoz/ency/plasma_renin_activity.jsp
Definition
Renin is an enzyme released by the kidney to help control the body's sodium-potassium balance, fluid volume, and blood pressure.
Purpose
Plasma renin activity (PRA), also called plasma renin assay, may be used to screen for high blood pressure (hypertension) of kidney origin, and may help plan treatment of essential hypertension, a genetic disease often aggravated by excess sodium intake. PRA is also used to further evaluate a diagnosis of excess aldosterone, a hormone secreted by the adrenal cortex, in a condition called Conn's syndrome.
Precautions
Patients taking diuretics, antihypertensives, vasodilators, oral contraceptives, and licorice should discontinue use of these substances for two to four weeks before the test. It should be noted that renin is increased in pregnancy and in diets with reduced salt intake. Also, since renin is affected by body position, as well as by diurnal (daily) variation, blood samples should be drawn in the morning, and the position of the patient (sitting or lying down) should be noted.
Description
When the kidneys release the enzyme renin in response to certain conditions (high blood potassium, low blood sodium, decreased blood volume), it is the first step in what is called the renin-angiotensin-aldosterone cycle. This cycle includes the conversion of angiotensinogen to angiotensin I, which in turn is converted to angiotensin II, in the lung. Angiotensin II is a powerful blood vessel constrictor, and its action stimulates the release of aldosterone from an area of the adrenal glands called the adrenal cortex. Together, angiotensin and aldosterone increase the blood volume, the blood pressure, and the blood sodium to re-establish the body's sodium-potassium and fluid volume balance. Primary aldosteronism, the symptoms of which include hypertension and low blood potassium (hypokalemia), is considered "low-renin aldosteronism."
Renin itself is not actually measured in the PRA test, because renin can be measured only with great difficulty even in research laboratories. In the most commonly used renin assay, the test actually determines, by a procedure called radioimmunoassay, the rate of angiotensin I generation per unit time, while the PRC (plasma renin concentration) measures the maximum renin effect.
Both the PRA and the PRC are extremely difficult to perform. Not only is renin itself unstable, but the patient's body position and the time of day affect the results. Also, the sample must be collected properly: drawn into a chilled syringe and collection tube, placed on ice, and sent to the performing laboratory immediately. Even if all these procedures are followed, results can vary significantly.
A determination of the PRA and a measurement of the plasma aldosterone level are used in the differential diagnosis of primary and secondary hyperaldosteronism. Patients with primary hyperaldosteronism (caused by an adrenal tumor that overproduces aldosterone) will have an increased aldosterone level with decreased renin activity. Conversely, patients with secondary hyperaldosteronism (caused by certain types of kidney disease) will have increased levels of renin.
Conn syndrome? I don't want that, either! I just want a normal, healthy life for a few years. AARRGGHH.
Thursday, October 9, 2008
Another blog mentions Cushing's
From the blog at http://fealubryne.livejournal.com/44195.html
...There's still the chance that things might not go as I'd like them. My medical record is a big red mark against me, and I may or may not be able to join because of it. I've gotten a number of iffy responses on the subject, though the recruiter I'm working with seems fairly confident that all I'll need is written off by an endocrinologist and I'll be fine, since I'm not currently displaying symptoms and I'm not on medication or anything because of it. So we'll see on that. In the mean time, however, my gallbladder definitely disqualifies me, but I'm having that out November 21st, and after the post-surgery waiting period I'll be otherwise sound of body and able to actually enlist when I get a yes or no on the Cushing's thing....
Wednesday, October 8, 2008
Does this disease make me look fat?
From http://calcitrix.livejournal.com/79399.html
For those of you new to my medical rambles, or needing a "previously on..."
I get vertigo, ear pain, headaches. My entire list of tests/things that have been tested for:
Glucose tolerance/diabetes
Hyper/hypo thyroid
Iron levels/other various things in the blood
Sinus/ear infections
Meniere's Disease
Benign Paroxysmal Positional Vertigo
Brain tumor (CT scan)
Tumor in the sinus cavity (CT scan)
Epilepsy/partial seizures (EEG)
Brain tumor (MRI)
Aneurysm (MRI)Those were all normal. So yesterday I had a spinal tap. It wasn't as horrific as I thought it would be, in that it didn't hurt. But it was very much like getting a tooth drilled--it didn't hurt, but I could feel the pressure, and it was very, very disturbing. Ick.
So...they measured the intracranial pressure of my spinal fluid, and it was "elevated." I HAVE AN ACTUAL RESULT! Basically the cerebral fluid in my brain isn't draining or being re-absorbed properly, so I get "pressure" headaches that last for months at a time, and the pressure bleeds over into my ear canals, causing tinnitus, pain, and vertigo. It isn't official, because this is just what the doctor doing the spinal tap said, but he named it "pseudotumor cerebri." I still have to meet with my neurologist again, though.
So I looked up this condition, and basically it means that I have all the symptoms of a large brain tumor, but without the brain tumor. Instead of a tumor pushing against areas of my brain, my cerebral fluid is doing it. And on the various web sites, the first thing they name as a cause is being obese. Now...I'm no skinny minnie. But I'm a size ten, which I consider reasonable for a woman in her mid-thirties. I eat well, and my job involves lots and lots of walking and hiking and being outside. But one website, in the same sentence it used the word "obese," added the detail "at least 20% above ideal body weight."Hmmm...so...at 5'4", I'm guessing my "ideal" body weight is about 125. Which makes "obese," in their opinion, 150 pounds. Uh, yeah, I'm a little over that. Screw you.
ANYWAY, two things stand out about the results of the spinal tap. One is that it actually makes sense for me to be affected by traveling in a plane. I thought it was really weird that I seemed to be much worse after flying somewhere, but the high altitude would certainly affect me.Huh.
And looking up the causes of increased intracranial pressure didn't reassure me. "No brain tumor" sounds great, but if it's caused by Cushing's Disease, the underlying cause could be a tumor on the pituitary gland, adrenal gland, or in the lung. A tumor that releases hormones. Blearghch. Then there's all the stuff about going blind, which. Yeah.
But it could be one of those "for no apparent reason" things, and I'll get treated with medicine to make my brain pressure go down, and that will be the end of it.
So...end of chapter four. I see the neurologist in a week, and he'll tell me what's what.
And we still don't know
From http://kaydenslife.blogspot.com/2008/10/and-we-still-dont-know.html
So in July I saw my primary care doctor who said she thought I had a thyroid issue. She ran some blood test for thyroid plus a few others for "just in case". My hormonal blood work came back normal but my cortisol levels were elevated. Basically (if you didn't read the cortisol link), this means that my body thinks I am stressed out and elevates my blood pressure and stores all of my calories. This is a throwback to caveman years when if you were stressed it meant you might not be able to find adequate food/water/shelter. There are a number of reasons why your cortisol would be elevated but mostly it points to a BENIGN tumor on either your adrenal or pituitary gland, causing a miscommunication. This is called Cushing's Syndrome. Don't go too crazy reading about it because it will freak you out, or it did to me. So much so I had to call my grandmother to talk me down off of my "too much information cliff"!
My doctor ran a number of other tests and referred me to an Endocrinologist, who I saw today. He thinks I have early signs of both Cushing's Syndrome and a thyroid issue with an indicator being Grave's disease (does it look like I have bulgy eyes to you???!) All of these issues are in a wait and see situation. I have to be monitored over the next year to see what happens but since the likelihood is that we will catch whatever it is, in a VERY early stage, he isn't too worried.
He told me to try to bring my cortisol down with Yoga, Tai-Chi and by slowly ending my day rather than watching TV and falling asleep. He thinks if I have a restful night of sleep, my cortisol will lower.
So, even though we still don't know exactly what the issue is, we know what to look-out for and have a plan. I will keep up with my Yoga, start a new diet plan that will hopefuly help and just try to be stress free.... easy, right???
Tuesday, October 7, 2008
Minimally Invasive Pituitary Surgery.
From http://www.laryngoscope.com/pt/re/laryngoscope/abstract.00005537-200810000-00027.htm;jsessionid=LrgKQznH2f2WtgDRrcGQyng3Q7q1y6YYQpkXBGP2c1qr5jNbGrvT!-2060166207!181195629!8091!-1
ARTICLE LINKS:
Fulltext | PDF (1.7 M)
Minimally Invasive Pituitary Surgery.
Sinonasal
Laryngoscope. 118(10):1842-1855, October 2008.
Senior, Brent A. MD; Ebert, Charles S. MD, MPH; Bednarski, Karen K. MD; Bassim, Marc K. MD; Younes, Mahar MD; Sigounas, Dimitri MD; Ewend, Mathew G. MD
Abstract:
Objectives/Hypothesis: Surgical approaches to the pituitary have undergone numerous refinements over the last 100 years. The introduction of the endoscope and the advent of minimally invasive pituitary surgery (MIPS) have revolutionized pituitary surgery. This study aims to compile and evaluate outcomes of all of the MIPS performed at our institution.
Study Design: Retrospective, cases series of 176 consecutive patients undergoing MIPS.
Methods: Patient demographics, tumor characteristics, and intraoperative or postoperative complications for of 176 consecutive patients undergoing MIPS were complied. Statistical analysis for categorical variables and incidence across series were conducted using Pearson's [chi]2 test and Fisher's exact tests. Odd ratios were calculated to relate the discrete variables to outcomes and designing clinical prediction of risk.
Results: One hundred seventy-six patients who underwent 193 procedures. Pathologic evaluation revealed 147 of the tumors to be pituitary adenomas. Only one death occurred (mortality rate of 0.5%). The rate of diabetes insipidus occurred in 20.2% of the procedures. Vascular complications occurred in 5.2% of the procedures. Intraoperative cerebrospinal fluid (CSF) leaks were identified in 19.7% whereas postoperative CSF leak was noted in 10.3%. Resection of Rathke's cleft cyst correlated higher risk of both intraoperative and postoperative CSF leak (OR = 2.6, P <.001). Resection of tumors other than adenomata correlated with significantly higher risk of CSF leak (OR = 9.0, P = <.001). Sinusitis occurred after eleven resections (5.7%). Meningitis occurred in 2 of 193 resections (1.0%) in our series. Two neurologic complications occurred in our series, pneumocephalus and cranial neuropathy (1.0%). No other complications occurred.
Conclusions: MIPS is a safe and efficacious marriage of the endoscope to the transsphenoidal approach. Thus, a brightness and clarity of vision is combined with the unique ability to explore the tumor bed with angled views and hydroscopy. Outcomes and complication rates comparable to traditional transsphenoidal approaches have resulted but with less dissection and tissue manipulation, reduced need for packing, and greater patient comfort and acceptance.
(C) The American Laryngological, Rhinological & Otological Society, Inc.
Sunday, October 5, 2008
It's Almost Endo Time Again
This Thursday I go back to Johns Hopkins for my annual post-Cushing's checkup. I used to go twice a year when I was on growth hormone but thanks to the cancer I can't take GH anymore.
I hope to have the courage to ask my endo for a script for Provigil. Dr. Dori mentioned it to me before an online interview and it sounds like something that would work for me.
But I don't know, if I get the script, if my kidney surgeon would let me take it. He's very protective of my one remaining kidney. I still wonder, though. If I took one pill, how much kidney "life" would I lose. Would it be worthwhile to gain a day of wakefulness and energy to lose an hour of kidney time?
At this stage of my life, I think that the trade off would be worthwhile. Of course, that's easy to say now. I'd probably feel different if I were undergoing dialysis!
But my endo might not even prescribe it so this may all be a wasted argument, even with myself.
Endocrinologist Dr. Jerald Marifke joins College faculty, Froedtert staff
from http://www.mcw.edu/display/docid396/NewsCenter/CollegeWeeklyNews/Endocrinol10.htm
Oct. 2, 2008 College News - Jerald Marifke, MD, has been appointed Assistant Professor of Medicine (Endocrinology, Metabolism and Clinical Nutrition) at the Medical College and to the medical staff of Froedtert Hospital. Board-certified in endocrinology, his clinical interests include evaluation and management of male hypogonadism, which is due to low testosterone. He also treats many endocrine disorders, including thyroid, adrenal and pituitary diseases.
Dr. Marifke comes to the Medical College from Endocrinology Associates of Green Bay, where he was a general adult endocrinologist in private practice. He completed an endocrinology fellowship at the University of North Carolina at Chapel Hill in 2000, where his research focused on patients with diabetes.
He served an internal medicine residency and internship at the Medical College in 1997 and 1995, respectively. He received his medical degree from the Medical College in 1994, and his bachelor of science, with honors, from the University of Wisconsin – Milwaukee in 1991.
Saturday, October 4, 2008
Bitemporal hemianopia
From http://internalmedicinemrcp.blogspot.com/

When I was in UK, I attended a PACES course. There were 3 patients whom I was asked to examine the visual fields and the findings were bitemporal hemianopia. They also had a scar as shown above. In fact, they had craniopharyngioma which has been operated via a transfrontal approach. You don't always get a clear scar like this in the exam. So, sometimes you have to look in between the hairs for the scar.
Where is the lesion ? Optic chiasm 
If you are asked to examine the eyes,
1) Inspection for scars (transfrontal and transphenoidal)
2) Examine the visual acuity with a Snellen chart
3) Test the visual fields (you will find bitemporal hemianopia)
4) Check light reflex and look for RAPD(relative afferent pupillary light reflex or Marcus Gunn pupil), accomadation reflex
5) Check eye movements
6) Do a fundoscopy ( look for optic atrophy, particularly if there is RAPD)
7) Look for a medic alert bracelet
8) Look for other features of endocrinopathy eg acromegaly, Cushing's syndrome which should also have been picked up during inspection
The other causes of a chiasmal lesion include pituitary adenoma, meningioma, aneurysm, glioma
Cushing’s Disease Causes Abnormal Growth
From http://www.cancerwise.org/September_2008/
Cushing’s Disease Causes Abnormal Growth
By Dawn Dorsey
A mother usually feels a sense of pride when she notices her child is growing. But Belinda Rivers knew something was wrong when her third-grader, Kevin, started to outgrow school-uniform pants as fast as she could buy them.
He gained 30 pounds in a year, but his appetite had not changed.
“The way he was eating just didn’t justify his weight gain, and he’s so active,” she says. “I knew kids had growth spurts, but this was ridiculous.”
Her intuition turned out to be right when Kevin was diagnosed with Cushing’s disease, a condition caused by a noncancerous tumor on the pituitary gland, the pea-shaped gland located at the base of the brain that controls the production of hormones. It also secretes growth hormone, which is responsible for growth in children and metabolic function in adults.
Weight gain is one of the primary symptoms of Cushing’s disease.
Weight began to balloon
Kevin’s pituitary tumor was causing the production of too much adrenocorticotropic hormone (ACTH). In turn, the ACTH stimulated the adrenal glands (which make steroid hormones and adrenaline). That led to an overproduction of cortisol and weight gain.
Despite the fact that he played football and baseball, Kevin quickly became overweight during his third-grade year. He went to an active outdoor camp and came back 10 pounds heavier. Then other kids started teasing him because of the extra pounds.
Belinda was at her wit’s end. Although Kevin had always been healthy and required only annual well-child pediatrician visits, they made a trip to the doctor. Belinda told him she knew something was wrong. Her trusted physician didn’t share her concern, however.
“He said, ‘Belinda, you and your husband are big people. He’s just big.’ But I knew something was wrong,” Belinda says. “I told him I wanted Kevin tested for everything.”
Her doctor referred Kevin to an endocrinologist (a physician who specializes in hormone disorders) in Slidell, La., close to where the Rivers family lives. Kevin’s blood and urine tests revealed high levels of cortisol, and a magnetic resonance imaging (MRI) test showed a tumor on his pituitary gland.
Photos told the story
When Belinda brought Kevin to M. D. Anderson, she was clutching two of Kevin’s baseball team photos: one from the year before his illness, one from the current year. She wanted to have proof in case anyone doubted there had been a dramatic change.
The photos were worth a thousand words to Steven Waguespack, M.D., associate professor in M. D. Anderson’s Department of Endocrine Neoplasia and Hormonal Disorders.
“Kevin had gained about 30 pounds in a year, but he had not grown any taller, which is very concerning for an underlying endocrine problem in children,” Waguespack says. “Weight gain around the middle is a classic symptom in adults, but in kids the weight gain is often distributed all over the body. That’s how it was with Kevin. However, he didn’t have some of the other classic symptoms of Cushing’s like muscle weakness, stretch marks or skin thinning.”
The type of tumor on Kevin’s pituitary was unusual as well. While most Cushing’s tumors are very small, often not visible even on an MRI, Waguespack says Kevin’s was large.
“Kevin is proof that every case of Cushing’s doesn’t always have classic symptoms,” Waguespack says.
Surgery provides a solution
Two weeks after Kevin's first visit to M. D. Anderson, Ian McCutcheon, M.D., a professor in M. D. Anderson’s Department of Neurosurgery who specializes in pituitary surgeries, removed Kevin’s tumor. The entire family traveled to Houston to be with him during his four-day hospitalization, and Kevin’s baby sister, Bailey, took her first steps at M. D. Anderson.
After surgery, Kevin was placed on steroids and thyroid replacement medication. He has since stopped taking the steroids, and Belinda expects the thyroid medicine will be stopped at his next checkup.
“He has been really brave,” Belinda says. “Sometimes right after the surgery he would say, ‘I think my tumor’s coming back.’ But we would tell him everything was OK and he would forget about it.”
Future filled with fun
It has been a year now since Kevin’s surgery. He’s 3 inches taller and has lost 18 pounds. Belinda says the mood swings that plagued him before surgery have disappeared.
Waguespack says Kevin’s future looks good.
“There’s always a chance of relapse with Cushing’s disease, especially when the tumor is large like Kevin’s,” he says. “But if a patient is going to relapse, it usually will happen within the first few years after surgery. If Kevin can make it five years, he will probably be OK.”
But Kevin doesn’t spend time worrying about it. He’s too busy playing any sport that comes along and racing his Christmas present/post-surgery treat: a brand-new dirt bike.
Related story:
Q&A: Cushing’s Disease and Cushing’s Syndrome
M. D. Anderson resources:
Adrenal Disease — Cushing’s syndrome